Learning Objectives
- Describe some of the main features and factors in the development of excoriation disorder
Excoriation disorder is an obsessive-compulsive spectrum disorder that is characterized by the repeated urge or impulse to pick at one’s own skin to the extent that either psychological or physical damage is caused.
Watch It
Watch this video to better understand the experience of living with a skin-picking disorder.
You can view the transcript for “What it’s like to have a skin-picking disorder” here (opens in new window).
Signs and Symptoms
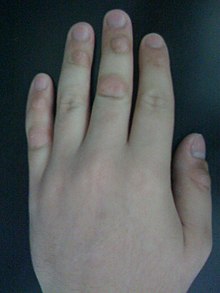
Figure 1. Compulsive picking of the knuckles (via mouth) illustrating potentially temporary disfiguration of the distal and proximal joints of the middle and little fingers.
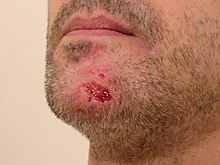
The region most commonly picked is the face, but other frequent locations include the arms, legs, back, gums, neck, shoulders, scalp, abdomen, chest, and extremities such as the fingernails, cuticles, and toenails. Most patients with excoriation disorder report having a primary area of the body that they focus their picking on, but they will often move to other areas of the body to allow their primary picking area to heal. Individuals with excoriation disorder vary in their picking behavior; some do it briefly multiple times a day while others can do one picking session that can last for hours. The most common way to pick is to use the fingers although a significant minority of people use tools such as tweezers or needles.
Skin picking often occurs as a result of some other triggering cause. Some common triggers are feeling or examining irregularities on the skin and feeling anxious or other negative feelings.
Complications arising from excoriation disorder include infection at the site of picking, tissue damage, and sepsis. Damage from picking can be so severe as to require skin grafting. Severe picking can cause epidermal abscesses. Severe cases of excoriation disorder can cause life-threatening injuries. For example, in one reported case, a female picked a hole through the bridge of her nose, which required surgery to fix, and a 48-year-old female picked through the skin on her neck exposing the carotid artery. Pain in the neck or back can arise due to prolonged bent-over positions while engaging in the behavior. Besides physical injuries, excoriation disorder can cause severe physical scarring and disfigurement.
Causes
There have been many different theories regarding the causes of excoriation disorder including biological and environmental factors. A common hypothesis is that excoriation disorder is often a coping mechanism to deal with elevated levels of turmoil, arousal, or stress within the individual, and that the individual has an impaired stress response. A review of behavioral studies found support in this hypothesis in that skin picking appears to be maintained by automatic reinforcement within the individual. In contrast to neurological theories, there are some psychologists who believe that picking behavior can be a result of repressed rage felt toward authoritarian parents. A similar theory holds that overbearing parents can cause the behavior to develop in their children.
Clinical studies have posited that there is a strong link between traumatic childhood events and excoriation disorder. Those with self-injurious disorders of the skin are found to also frequently report childhood sexual abuse. While attempting to produce diagnostic criteria for excoriation disorder, researchers conversed with 10 patients with the disorder and found that a majority reported personal problems before the picking began, and four reported on abuse they suffered in childhood or adolescence.[1]
Neurological
Studies have shown a linkage between dopamine and the urge to pick. Drugs such as cocaine and methamphetamine, which increase the pharmacological effects of dopamine, have been shown to cause uncontrollable picking in users. Central nervous system stimulants may create the sensation of formication, which feels like something is crawling on or under the skin. Thus, excoriation disorder could result from a dysfunction in the dopamine reward functions.

Figure 3. The anterior cingulate cortex, part of the right-lateralized frontostriatal circuit, is shown here. We know that it plays a role in motor-inhibitory control and may be associated with excoriation disorder.
There may be another neurological explanation for excoriation disorder: individuals with the condition have less motor-inhibitory control, but show no sign of difference in cognitive flexibility, when compared to individuals without the condition. Motor-inhibitory control is a function of the right-lateralized frontostriatal circuit, which includes the right inferior frontal and bilateral anterior cingulate cortices. The impairment of motor-inhibitory control is similar to the neurological conditions of those who have problems suppressing inappropriate behaviors, such as abusing methamphetamine.
Epidemiology
The prevalence of excoriation disorder is not well understood. Estimates of prevalence of the condition range from 1.4 to 5.4% in the general population. One U.S. telephone survey found that 16.6% of respondents “picked their skin to the point of noticeable tissue damage” and that 1.4% would qualify as meeting the requirements of excoriation disorder. Another community survey found a rate of 5.4% had excoriation disorder. A survey of college students found a rate of 4%.[2] One study found that among non-disabled adults, 63% of individuals engaged in some form of skin picking and 5.4% engaged in serious skin picking.[3] Lastly, a survey of dermatology patients found that 2% suffered from excoriation disorder. Excoriation disorder is statistically more common in females than in males.
In some patients, excoriation disorder begins with the onset of acne in adolescence, but the compulsion continues even after the acne has gone away. Skin conditions such as keratosis pilaris, psoriasis, and eczema can also provoke the behavior. In patients with acne, the grooming of the skin is disproportionate to the severity of the acne. Certain stressful events including marital conflicts, deaths of friends or family, and unwanted pregnancies have been linked to the onset of the condition. If excoriation disorder does not occur during adolescence, another common age of onset is between the ages of 30 to 45. Additionally, many cases of excoriation disorder have been documented to begin in children under the age of 10. One small survey of patients with excoriation disorder found that 47.5% of them had an early onset of excoriation disorder that began before age 10. Traumatic childhood events may initiate the behavior.
Coborbidity
Excoriation disorder has a high rate of comorbidity with other psychiatric conditions, especially with mood and anxiety disorders. One survey of patients with excoriation disorder found that 38% also had alcohol- or drug-abuse problems. Studies have shown the following rates of psychiatric conditions found in patients with excoriation disorder: trichotillomania (38.3%), substance abuse (38%), major depressive disorder (approximately 31.7% to 58.1%), anxiety disorders (approximately 23% to 56%), OCD (approximately 16.7% to 68%), and body dysmorphic disorder (approximately 26.8% to 44.9%). There are also higher rates of excoriation disorder in patients in psychiatric facilities; a study of adolescent psychiatric inpatients found that excoriation disorder was present in 11.8% of patients. It is also present at high rates with some other conditions: 44.9% of patients with body dysmorphic disorder also have excoriation disorder; 8.9% of patients with OCD have excoriation disorder; and 8.3% of patients with trichotillomania have excoriation disorder.
Excoriation disorder has been the subject of several episodes of Obsessed, a television documentary series that focuses on treatment of anxiety disorders. Skin picking is shown as a symptom of Nina Sayers’ anxiety and OCD in the movie Black Swan.
Key Takeaways: Excoriation Disorder
Link to Learning
Watch this Ted talk by artist Liz Atkin and listen to her tell her own story of struggle and recovery in dealing with excoriation disorder.
Try It
Glossary
excoriation disorder: an obsessive-compulsive spectrum disorder that is characterized by the repeated urge or impulse to pick at one’s own skin to the extent that either psychological or physical damage is caused
formication: the sensation of something that is crawling on or under the skin
Candela Citations
- Modification, adaptation, and original content. Authored by: Christina Hicks for Lumen Learning. Provided by: Lumen Learning. License: CC BY-SA: Attribution-ShareAlike
- Excoriation Disorder. Provided by: Wikimedia. Located at: https://en.wikipedia.org/wiki/Excoriation_disorder. License: CC BY-SA: Attribution-ShareAlike
- RI slice with highlighting indicating location of the anterior cingulate cortex. Authored by: Geoff B Hall. Provided by: Wikimedia. Located at: https://en.wikipedia.org/wiki/Anterior_cingulate_cortex#/media/File:MRI_anterior_cingulate.png. License: CC0: No Rights Reserved
- Body focused repetitive disorders (trichotillomania & excoriation). Provided by: Osmosis. Located at: https://www.youtube.com/watch?v=jFxoT3coHas. License: Other. License Terms: Standard YouTube License
- What it's like to have a skin-picking disorder. Provided by: Newsy. Located at: https://www.youtube.com/watch?v=5WYpRZbF1Jg. License: Other. License Terms: Standard YouTube License
- Yalçin M, Tellioğlu E, Yildirim DU, Savrun BM, Özmen M, Aydemir EH (December 2015). "Psychiatric Features in Neurotic Excoriation Patients: The Role of Childhood Trauma". Noro Psikiyatri Arsivi. 52 (4): 336–341. doi:10.5152/npa.2015.9902. PMC 5353104. PMID 28360736 ↵
- Odlaug BL, Grant JE (September 2010). "Pathologic skin picking". The American Journal of Drug and Alcohol Abuse. 36 (5): 296–303. doi:10.3109/00952991003747543. PMID 20575652 ↵
- Lang R, Didden R, Machalicek W, Rispoli M, Sigafoos J, Lancioni G, Mulloy A, Regester A, Pierce N, Kang S (2010). "Behavioral treatment of chronic skin-picking in individuals with developmental disabilities: a systematic review". Research in Developmental Disabilities. 31 (2): 304–15. doi:10.1016/j.ridd.2009.10.017. PMID 19963341 ↵