Infection in Urinary system:
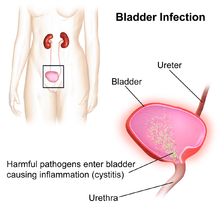
- Infection localized in the ureter is called urethritis. Urethritis is inflammation of the urethra. The most common symptom is painful or difficult, urination.
- If the infection spreads to urinary bladder, then it is called cystitis.
- If the kidneys are infected, it is called pyelonephritis
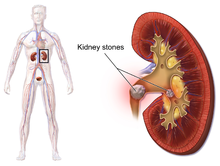
Kidney Stones
The kidney plays a very important role in the body as it filters out waste products. Sometimes kidney stones can form when there is a build up of specific minerals in your urine. Kidney stones are hard, pebble-like pieces of material that form in one or both of your kidneys. They rarely cause permanent damage if treated by a health care professional.
Kidney stones vary in size and shape. They may be as small as a grain of sand or as large as a pea. Rarely, some kidney stones are as big as golf balls. Kidney stones may be smooth or jagged and are usually yellow or brown. A small kidney stone may pass through your urinary tract on its own, causing little or no pain. A larger kidney stone may get stuck along the way. A kidney stone that gets stuck can block your flow of urine, causing severe pain or bleeding.
Polycystic Kidney Disease

Polycystic Kidney Disease
Polycystic kidney disease (PKD or PCKD, also known as polycystic kidney syndrome) is a cystic genetic disorder of the kidneys. There are two types of PKD: autosomal dominant polycystic kidney disease (ADPKD), and the less-common autosomal recessive polycystic kidney disease (ARPKD). PKD is characterized by the presence of multiple cysts (hence,”polycystic”), typically in both kidneys. The cysts are numerous and are fluid-filled, resulting in massive enlargement of the kidneys. The disease can also damage the liver, pancreas, and, in some rare cases, the heart and brain. The two major forms of polycystic kidney disease are distinguished by their patterns of inheritance. Polycystic kidney disease is one of the most common life-threatening genetic diseases, affecting an estimated 12.5 million people worldwide.
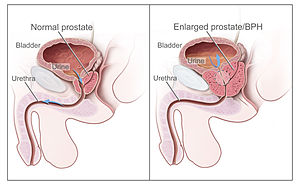
Benign Prostatic Hyperplasia (BPH)
The prostate is a walnut-sized gland of the male reproductive system between the bladder and the penis. The urethra runs through the center of the prostate. Benign prostatic hyperplasia (BPH), also called prostate enlargement, is a noncancerous increase in the size of the prostate gland. Symptoms may include frequent urination, trouble starting to urinate, weak stream, inability to urinate, or loss of bladder control. Complications can include urinary tract infections, bladder stones, and chronic kidney problems.
Renal Failure
Many illness can cause progressive renal diseases and renal failure, especially diabetes and hypertension. Renal failure (also kidney failure or renal insufficiency) is a medical condition in which the kidneys fail to adequately filter waste products from the blood. Diagnosis: Renal failure is mainly determined by a decrease in the glomerular filtration rate, which is the rate at which blood is filtered in the glomeruli of the kidney. This is detected by a decrease in or absence of urine production or determination of waste products (creatinine or urea) in the blood. Depending on the cause, hematuria (blood loss in the urine) and proteinuria (protein loss in the urine) may be noted.
In renal failure, there may be problems with increased fluid in the body (leading to swelling), increased acid levels, raised levels of potassium, decreased levels of calcium, increased levels of phosphate, and in later stages, anemia. Bone health may also be affected. Long-term kidney problems are associated with an increased risk of cardiovascular disease.
Categories of Renal Failure
Renal failure can be divided into two categories: acute kidney injury or chronic kidney disease .The type of renal failure is determined by the trend in the serum creatinine. Other factors that may help differentiate acute kidney injury from chronic kidney disease include anemia and the kidney size on ultrasound. Chronic kidney disease generally leads to anemia and small kidney size.
Acute kidney injury (AKI), previously called acute renal failure (ARF), is a rapidly progressive loss of renal function, generally characterized by oliguria (decreased urine production, quantified as less than 400 mL per day in adults, less than 0.5 mL/kg/h in children or less than 1 mL/kg/h in infants); and fluid and electrolyte imbalance. AKI can result from a variety of causes, generally classified as prerenal, intrinsic, and postrenal. An underlying cause must be identified and treated to arrest the progress, and dialysis may be necessary to bridge the time gap required for treating these fundamental causes.
Chronic kidney disease (CKD) can also develop slowly and, initially, show few symptoms. CKD can be the long-term consequence of irreversible acute disease or part of a disease progression.
Symptoms can vary from person to person. Someone in early stage kidney disease may not feel sick or notice symptoms as they occur. When kidneys fail to filter properly, waste accumulates in the blood and the body, a condition called azotemia. Very low levels of azotaemia may produce few, if any, symptoms. If the disease progresses, symptoms become noticeable (if the failure is of sufficient degree to cause symptoms). Renal failure uremia is a syndrome of renal failure characterized by elevated levels of urea and creatinine in the blood.
Renal Failure Uremia
Renal failure uremia is a syndrome of renal failure that includes elevated blood urea and creatinine levels. Acute renal failure can be reversed if diagnosed early. Acute renal failure can be caused by severe hypotension or severe glomerular disease. Diagnostic tests include BUN ( Blood Urea Nitrogen ) and plasma creatinine level tests. It is considered to be chronic renal failure if the decline of renal function is to less than 25%.
If you catch kidney disease early, you may be able to prevent kidney failure by taking steps to keep your kidneys as healthy as possible for as long as possible. If your kidneys fail, you will need dialysis or a kidney transplant to survive.
Hemodialysis/dialysis is a process of purifying the blood of a person whose kidneys are not working normally. Dialysis removes excess fluid, correct electrolyte problems, and remove toxins in those with kidney failure, thus maintaining homeostasis.
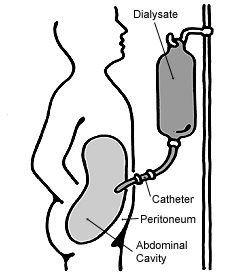
During hemodialysis, patient’s blood is pumped through a filter, called a dialyzer. This machine works like an artificial kidney and filters out extra salt, waste, and fluid. Cleaned blood is sent back into your body through the second needle. Peritoneal dialysis (PD) uses the peritoneum in a person’s abdomen as the membrane through which fluid and dissolved substances are exchanged with the blood.
Kidney Transplantation
Kidney transplantation is the organ transplant of a kidney into a patient with end-stage renal disease. The transplanted kidney takes over the work of the two kidneys that failed, so you no longer need dialysis. Kidney transplantation requires a person to be at the end stage of renal failure.

Kidney Transplantation